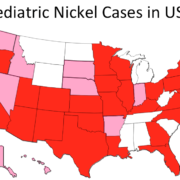
A Serious ‘Tipping Point’ – Demand for allergic contact dermatitis specialists by sufferers far exceeds supply

This is Francine’s story, written from the perspective of her allergic contact dermatitis provider (contact dermatologist), Dr. Sharon Jacob. Together the patient and provider worked together to properly evaluate her through patch testing which gave Francine her life back by helping to resolve her allergic contact dermatitis.
Anger, sheer anger, “How can we have to wait 11 months to see the doctor? Tell her my son is suffering, tell her I can not live seeing my child live like this.”
I would like to introduce you to Francine.* She was an ex-cosmetic fragrance counter worker, who had to quit her job because of rashes. She came referred from her 4th dermatologist who wanted to start cyclosporine (an immunosuppressive medicine used to prevent transplant rejection) but she couldn’t afford the medication. I looked into her eyes, her eyelids so inflamed they were peeling back. She was suffering from allergic contact dermatitis. She asked “can you get me better?” I humbly said, “I am surely going to try”, and swore to myself that I would not take hope from this patient.
We patch tested her to balsam of Peru (BOP) and the individual BOP components and confirmed she was highly allergic to cinnamate derivatives and benzyl alcohol. Unfortunately, her current topical medication contained benzyl alcohol. (1) We instituted avoidance and she dramatically improved. She told me “Patch testing gave me my life back”. Three months later she ‘cheated with a cinnamon bun at the mall and had a severe flare that led her back to my office. We reviewed that avoidance is the permanent treatment for allergic contact dermatitis.
Before:
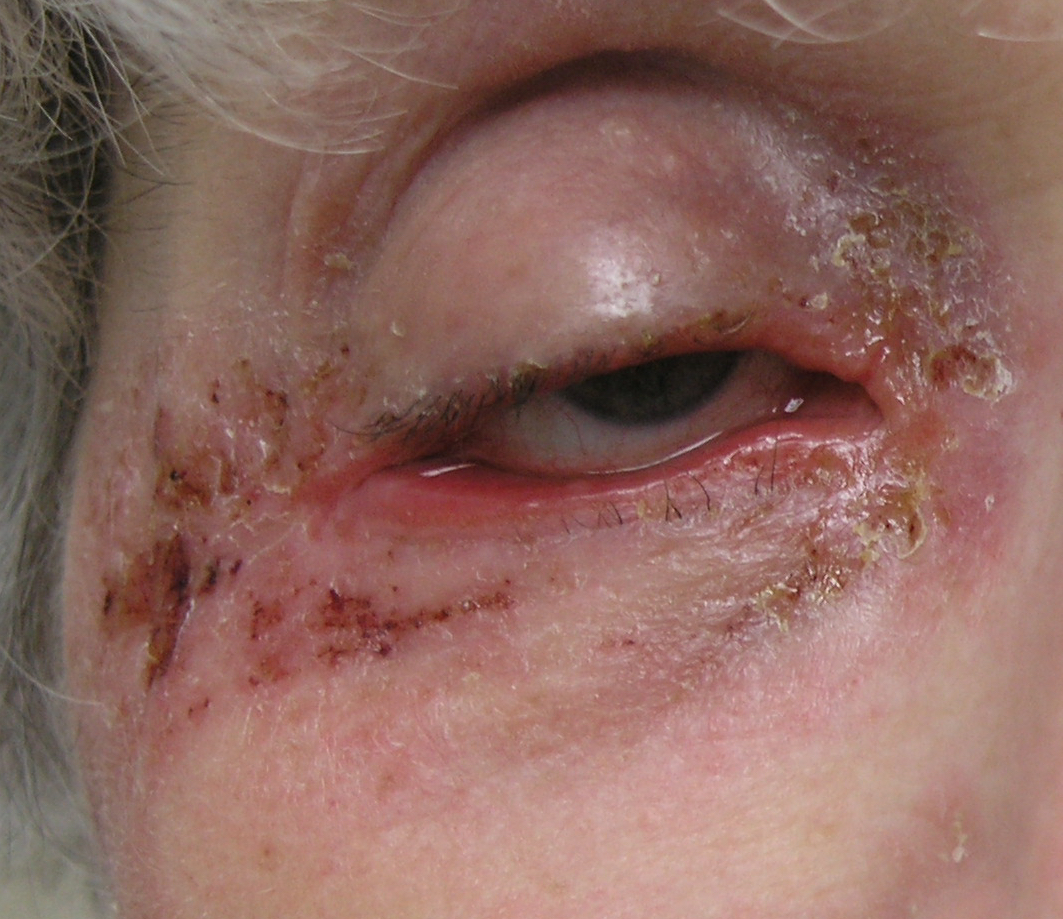
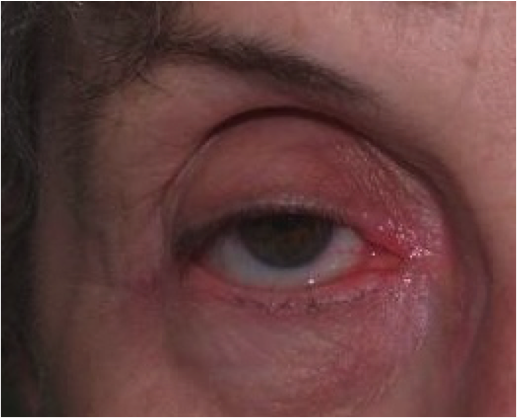
After:
Five minutes later, I looked into the eyes of the next patient’s distraught father. He raised his voice at me, frustrated that they had to wait so long. “We just can’t understand why you just couldn’t put our son in. Look at him, he has worsened waiting for you. Look at him”. Do I tell them I haven’t regularly eaten lunch in 3 years, do I tell them that this epidemic has caused me to cut routine sleep out of my daily life. No.
“I am sorry”, I say, “I am here to help, but anger fills the room. We do the evaluation to determine if patch testing is appropriate and then I tell them we will schedule their patch test appointment. “What, you are going to make me wait again?” “What is wrong with you?” I explain we do custom tailored patch tests and we now have to make them by hand for their son. Dad points at the nurse who has come in to tell me that the next roomed patient is now delayed, and we have three walk-ins in the waiting room pleading to be seen. I gently ask the nurse to tell the next patient I will be right there. Dad takes his son by the hand and storms out. I am beside myself. The desperate child looks back at me with sorrowful eyes (the first deliberate-eye contact of the appointment) – my heart breaks.
There are days when the graduates’ hugs are far more needed by me, than by them. (Graduates are the people who have learned their allergens, avoided them, regained control of their lives becoming rash free and informed.)
Unfortunately, it was the ‘same’ story every 30 minutes of my contact dermatitis work life. Nickel, balsam of Peru, formaldehyde, methylchloroisothiazolinone, cocamidopropyle betaine… yes there are also new emerging allergens, but if formaldehyde has been on Bonneville’s bad list for over 80 years, why are we not doing something about it? The answer was not to keep seeing the 1000s, but to reach the millions.
We formed the Dermatitis AcademyTM to reach the patients, reach the providers and grow hope in reaching the legislators. www.dermatitisacademy.com
The unmet need – supply and demand:
How many tertiary care centers in the US are dedicated primarily to patch testing? Now that is a good question!
The largest multicenter group of 15 dermatologists, the North American Contact Dermatitis Group tested 4,238 patients in 2011-2012 cycle, ~280 per provider). (2)
An estimated 60% of the members of the American Contact Dermatitis Society (ACDS) do comprehensive patch testing. In dermatology private practice, 83% of practitioners patch test fewer than 5 patients/month. (3,4) Guestimating (and a likely overestimate) 150 centers nationally patch testing 50% of the time estimates 280 x 150 = 42,000 patients potentially being tested each year. If 80 million people are suffering with contact dermatitis (the prevalence rates are believed to be 24,400 cases per 100,000 individuals/yr) and only 42k are being provided with patch testing, then there is a huge unmet need for the diagnostic evaluation of allergic contact dermatitis. This deficit leads to high morbidity (conditions difficult to live with) and huge direct and indirect expenses (associated with allergic contact dermatitis) to the health care system (in the Billions). (5)
This best multi-faceted solution to the burden of skin disease caused by allergic contact dermatitis is routed in appropriate patch testing, appropriate access to properly trained providers, outreach in education for prevention and evidence-based safety regulation in manufacturing.
1) Jacob SE. Ciclosporin emulsion a novel treatment for benzyl alcohol associated eyelid dermatitis. Contact Dermatitis. 2008. 58: 169-170.
2) Warshaw EM, Moore JB, Nelson D. Patch-testing practices of ACDS members: a cross-sectional Survey. Am J Contact Dermatol 14:5-11, 2003
3). Scheman A. et al. Patch Testing An Underutilized Modality. Arch Dermatol 140: 1529-30, 2004
4) Warshaw EM, Maibach HI, Taylor JS, Sasseville D, DeKoven JG, Zirwas MJ, Fransway AF, Mathias CG, Zug KA, DeLeo VA, Fowler JF Jr, Marks JG, Pratt MD, Storrs FJ, Belsito DV. North American contact dermatitis group patch test results: 2011-2012. Dermatitis. 2015 Jan-Feb;26(1):49-59.
5) Bickens DR, et al. The burden of skin diseases: 2004 a joint project of the American Academy of Dermatology Association and the Society for Investigative Dermatology. J Am Acad Dermatol. 2006 Sep;55(3):490-500.
*names changed to protect the patient



 Photo by Retha Ferguson from Pexels
Photo by Retha Ferguson from Pexels